A study on sleep architecture in patients with chronic respiratory failure under long-term oxygen therapy—Focused on the influence of ventilatory failure (high CO2) elements on the patient’s sleep architecture ()
1. INTRODUCTION
The goal of Long-Term Oxygen Therapy (LTOT) or Home Oxygen Therapy is to improve respiratory failure in patients with Chronic Respiratory Failure (CRF) and heart failure, which are defined by the partial pressure of arterial oxygen (PaO2), through maintaining a certain oxygen level at rest and during exertion and sleep [1-3]. Accordingly, application of the therapy and oxygen dosage is usually determined based on the PaO2 at rest and in accordance with the evaluation of PaO2 during exertion and sleep [4]. However, patients under LTOT often experience aggravation of the respiratory status of which the cause is sometimes not identified.
Many of such patients are hospitalized and discharged repeatedly without being given any novel treatment resulting in the term in which oxygen administration alone cannot maintain the condition and artificial ventilation is required in an intensive care unit.
We noticed that CRF patients under LTOT who experience repeated acute aggravation regardless of hypoxemia resolution with oxygen therapy tend to request a hypnotic prescription and complain of insomnia.
Patients with COPD who need LTOT tend to have insomnia and sleepiness during the daytime in addition to a higher incidence of nightmare compared to healthy subjects [5,6]. Insomnia, early morning awakening and daytime drowsiness are also observed in asthmatic patients not necessarily with respiratory failure [7]. We sometimes have no choice but to prescribe hypnotics for respiratory failure patients who complain of insomnia. Although some studies [7] report that recent hypnotics are relatively safe for use in respiratory failure patients, most hypnotics and sedatives have some muscle relaxant and respiratory depression actions [8-12]. Therefore, hypnotics for sleep improvement should be administered carefully in CRF patients who complain of insomnia and tend to have daytime drowsiness. For safe and rational treatment, it is essential to understand the sleep state in respiratory failure patients without the use of any agent that could influence sleep. And many studies have shown that hypoxemia during sleep causes arousal response and that sleep stages are associated with aggravation and improvement of hypoxemia in respiratory failure patients [13-16].
However, there are few sleep-physiological studies regarding the influence of respiratory disorder on sleep state in chronic respiratory failure patients, especially, the influence of such disorder on the sleep architecture in CRF patients under LTOT. Although one report [17] on the influence of ventilatory failure and hypercapnia on sleep in healthy subjects has been published, the influence on sleep in patients with CRF is yet to be revealed.
We evaluated the sleep architecture in CRF patients under LTOT using polysomnography (PSG) including electroencephalogram, investigated the clinical conditions of the patients focusing on the influence of hypercapnia on sleep architecture, and presented the findings below.
2. PATIENTS AND METHOD
2.1. Subjects
The subjects were 13 male CRF patients of the Respiratory Division in Hachinohe Red Cross Hospital (8 patients with COPD, 2 patients with [diffuse panbronchiolitis]; DPB, 1 patient with [interstitial pneumonitis]; IP, and 2 patients with [Rheumatoid]; RA lung), all of whom are under LTOT. The oxygen dosage for each patient was determined thorough blood gas analysis at rest, SpO2 measurement during sleep, and 12 minutes walking test. The controls were 7 male healthy subjects without any findings of sleep disturbance and respiratory failure under PSG, who are outpatients of the Respiratory Division in Hachinohe Red Cross Hospital and matched by gender and age. All the subjects gave written informed consent for using the test results during hospitalization for scientific research. And this study approved by IRB of Hachinohe Red Cross Hospital.
2.2. Polysomnography and Arterial Blood Gas Analysis during Wakefulness
An overnight full-montage polysomnogram was carried out in accordance with the current standards of the American Academy of Sleep Medicine (AASM) [17]. All subjects did not take any xanthine-contained medicine, hypnotics and sedatives in the day of this investigation. The sleep study was started at 8:00 pm and completed at 6:00 am on the following day. The recording montage consisted of continuous recordings of the following physiologic channels: C3-A2 and C4-A1 electro-encephalogram (EEG), right and left electro-oculogram (EOG), a single bipolar electrocardiogram (ECG), chin electromyogram (EMG), oxyhemoglobin saturation by pulse oximetry, chest and abdominal excursion by inductance plethysmography, airflow by an oronasal thermocouple, and body position by a mercury gauge. Scoring of the sleep data were conducted as follows. Initially, an automated computerized analysis of sleep and breathing abnormalities was performed using the Allis Sleepware v. 2.7.43 (Philips Respironics) program. Then, a trained sleep technician and a sleep physician visually assessed and corrected the data in accordance with the current standards of sleep and respiratory scoring.
Radial arterial blood was collected after the subjects were maintained at rest in the supine position for 1 hour with oxygen supplied at the time of admission and the specimens were analyzed using an arterial blood gas analyzer (ABL 700 series, Radiometer, Copenhagen, DK).
2.3. Calculation of Baseline PaCO2
The ABG obtained from the blood collected at the time of admission is the data during wakefulness. Assuming that bicarbonate ion ( ) concentration derived from the ABG data reflects CO2 at rest based on the Henderson-Hasselbalch equation and that the concentration includes PaCO2 during sleep, PaCO2 at rest includeing during sleep was estimated using the following prediction Formula (1) [18].
) concentration derived from the ABG data reflects CO2 at rest based on the Henderson-Hasselbalch equation and that the concentration includes PaCO2 during sleep, PaCO2 at rest includeing during sleep was estimated using the following prediction Formula (1) [18].
 (1)
(1)
Since ventilation is generally suppressed during sleep, ventilatory status during sleep is considered to be an important influential factor affecting the value obtained by the above Formula (1).
2.4. Statistical Analysis
Regarding analysis of the data on the LTOT and Control Groups, the three groups were compared using ANOVA. In regard to analysis of the data on the High CO2 Group and the Normal CO2 Group, Cochran-cox test was used.
3. RESULTS
Table 1 shows the demographics and PSG data on each subject group (Table 1). Significant differences

Table 1. Clinical characteristics of control subjects and patients of LTOT (mean ± S.E.).
were found between the LTOT and Control Groups regarding Total Sleep Time (TST), Sleep Efficiency (SE), % stage 1 (N1), % stage 3 + 4 (N3), and % stage REM(R). The values were 288.1 ± 31.8 mins, 45.6% ± 3.5%, 30.9% ± 5.5%, 0.1% ± 0.1%, and 18.8% ± 2.0%, respecttively, in the LTOT Group (mean ± S.E.) while they were 388.1 ± 15.7 mins, 72.7% ± 2.8%, 26.3 ± 1.6, 8.3% ± 3.4%, and 10.1% ± 2.3% (mean ± S.E.), respectively, in the Control Group. TST, SE, and % stage 3 + 4 (N3) were significantly lower (P < 0.05, P < 0.0001, P < 0.005) while % stage 1 (N1) and % stage REM (R) were significantly higher (P < 0.05, P < 0.05) in the LTOT Group. Sleep latency (SL) was 76.9 ± 16.0 mins in the LTOT Group and significantly higher (P < 0.05) than that of the Control Group, which was 25.2 ± 4.8 mins (Figures 1 and 2).
Regarding the other PSG parameters, Arousal and Apnea hypopnea indices were significantly higher in the LTOT Group (P < 0.05 and P < 0.05): 17.5 ± 2.1 times/hour vs. 11.3 ± 2.3 times/hour and 14.4 ± 3.9 times/hour vs. 1.9 ± 0.6 times/hour.
In comparison of the 6 LTOT patients with elevated baseline PCO2 (PCO2 ≥ 45) (Hypercapnia: H Group) and 7 patients with normal baseline PCO2 (PCO2 < 45) (Normocapnia: N Group) matched by age, hypoxemia (SpO2 < 90%) was not observed during sleep in both groups and SL was significantly higher (P < 0.01) in the H Group: 123.8 ± 18.8 mins in the H Group vs. 36.7 ±

Figure 1. Total sleep time (TST), Sleep Efficiency and Sleep Latency of the PSG data in 7 control subjects and 13 LTOT subjects mean ± SE. †P < 0.05, *P < 0.0001.

Figure 2. Stage N1, Stage N2 and Stage R of the PSG data in 7 control subjects and 13 LTOT subjects mean ± S.E. †P < 0.05, ‡P < 0.005.
10.9 mins in the N Group. TST, SE, N1, N2, N3, and R did not differ significantly between the two groups (Figure 3, Table 2).
Although it is noteworthy that Periodic leg movement disorder (PLMD) was observed in 62.5% of the LTOT patients with especially high PLMD complication incidence of 50% in the H Group, but there was no correlation of this finding to sleep interruption (Figure 4).
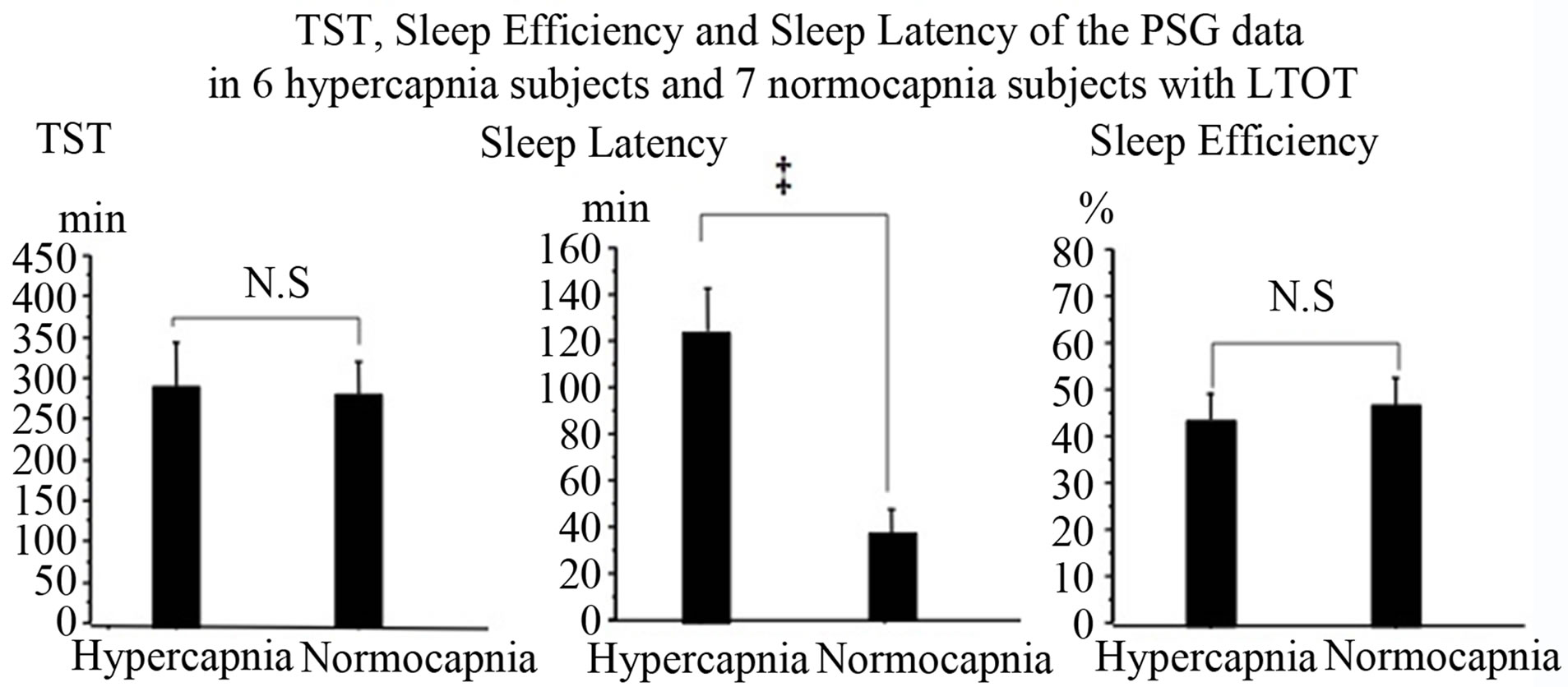
Figure 3. Total sleep time (TST), Sleep Efficiency and Sleep Latency of the PSG data in 6 hypercapnia subjects and 7 normocapnia subjects with LTOT mean ± SE. ‡P < 0.005.
4. DISCUSSION
CRF in patients is usually diagnosed based on clinical definitions, which are all based on the presence of hypoxemia and categorized depending on whether being accompanied by hypercapnia [19-21]. This means that all CRF patients have hypoxemia and that the study needs to be conducted with the influence of hypoxemia excluded by the means of oxygen administration.

Figure 4. A ratio of PLMD of 7 contral subjects, 6 hypercapnia subjects with LTOT, 7 Normocapnia with LTOT and 13 LTOT with LTOT.

Table 2. Clinical characteristics of control subjects and patients of hypercapnia and normocapnia with LTOT (mean ± S.E.).
Accordingly, the primary endpoint of this study was to investigate the influence of chronic hypercapnia in patients with hypoxemia resolved by means of LTOT.
In order to compare the influence of respiratory failure in hypoxemia and ventilatory failure patients under LTOT, baseline PaCO2 values that reflect the ventilatory state during sleep were derived from the bicarbonate ion (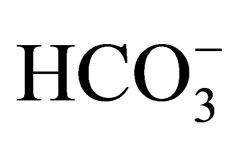 ) values using the prediction formula [18].
) values using the prediction formula [18].
This is based on the fact that PaCO2 becomes higher due to the physiological suppression of ventilation during sleep. In addition, PaCO2 values at wakefulness do not reflect the values during sleep. Thus, we derive the baseline PaCO2 during sleep from  that reflects longer-term PaCO2 and needs prolonged period to change.
that reflects longer-term PaCO2 and needs prolonged period to change.
Assuming that the predicted PaCO2 at rest reflects PaCO2 during sleep, the LTOT patients were categorized by the level of PaCO2 during sleep and PSG data for each group were compared.
Regarding nocturnal sleep architecture in CRF patients under LTOT, it was characterized by shorter TST, larger % stage N1, smaller % stage N3, and longer sleep latency, namely, lower sleep efficiency compared to healthy subjects even with the maintenance of oxygen level during sleep by means of oxygen administration.
These characteristics are evidences of so-called sleep disturbance of which the pattern was different from the pattern attributable to certain events and accompanied by arousal responses such as observed in obstructive sleep apnea hypopnea syndrome (OSAHS). Rather, it was similar to have sleep architecture in sleep disturbance observed in generalized anxiety disorder. Although some studies report that high PaCO2 is responsible for arousals [22], a causal relationship between high PaCO2 and arousals was not found in LTOT patients. Future studies may reveal such causal-relationship through long-term follow up of sleep variation in respiratory failure patients. This study probably failed to prove the association of high PaCO2 with arousals due to a lack of sleep tests in matched patient groups before the patients contracted respiratory failure. When hypercapnia and normocapnia patients in the LTOT Group were compared, sleep latency was shorter in hypercapnia patients. The influence of PaCO2 was considered to be one of the causes.
In patients classified into the LTOT Group, PLMD complication incidence was around 50% with no relation to PaCO2 accumulation.
Regarding insomnia related to respiratory diseases, there are many reports on bronchial asthma [7,18]. COPD patients present various symptoms depending on the disease types and severity. The most frequent symptom in patients at Stage 2 or higher is “exertional dyspnea” while severe breathing difficulty that interrupts sleep at night is rare unless accompanied by bronchial asthmatic attack [23] or accidental pneumothorax.
Pulmonary emphysema at the stationary phase rarely causes insomnia because it is rarely accompanied by symptoms of cough and sputum. Significant hypoxemia during REM sleep associated with decrease in PaO2 partial pressure during wakefulness is reported regarding sleep in COPD patients [24].
However, there are no reports on sleep state in LTOT patients. We found in this study that sleep in LTOT patients is characterized by shorter TST, larger Stage N1, longer sleep latency and lower sleep efficiency compared to controls. These characteristics are similar to the sleep pattern in patients with generalized anxiety disorder.
Regarding the subjects in this study, in whom normal oxygen saturation is maintained during sleep by means of oxygen administration, possible causes of sleep disturbance are biological and physical stressors such as respiratory muscle fatigue and factors related to anxiety disorders due to slow aggravation of the ventilatory state.
Guilleminalt [25] et al. first reported the incidence of PLMD in sleep disorder and revealed that PLMD was observed in 11.3% of chronic insomnia patients. Colemen [26] et al. reported that PLMD was observed in 3.5% of hypersomnia patients and this incidence was raised to 18% in such patients aged 65 or over. Since the incidence of PLMD is high in the patients with cerebrovascular disorder and myelopathy, damage to the inhibitory system between the central nerve and ventral horn cell that functions during sleep may be associated with decrease in the threshold of the disease onset [27]. Variance in sympathetic nerve activity in the pons and reticular formation seems to be associated with periodic onset of PLMD since the interval of muscle contraction matches the fluctuation of breathing, arterial and cerebrospinal fluid pressure, which is suppressed by sympathetic nerve system during sleep [28]. No healthy subjects in this study were diagnosed as having PLMD based on the PSG data, probably due to the small number of the cohort. On the other hand, PLMD was found in 62.5% of the LTOT patients although the number of the cohort is so small. Studies with a larger number of cohorts may be required in the future.
Respiratory disease, especially COPD, has been considered to be a cause of insomnia since the incidence of insomnia is higher in patients with this disease compared to healthy controls [29]. Many studies in the past investigated the sleep state before commencement of LTOT. In addition to this, we classified patients depending on whether they had hypercapnia and compared the differences in sleep state among the groups. We supposed that frequent measurements of nocturnal oxygen concentration during sleep could affect sleep testing and insertion of the Swan-Ganz catheter for testing presents high risk to the LTOT patients. Therefore, assuming that the predicted PaCO2 derived from the value of , which is obtained from the ABG analysis of the blood collected at the time of admission while the patient is awake, reflects the PaCO2 during sleep, we estimated the PaCO2 level during sleep using the prediction formula for PaCO2 at rest including during sleep (
, which is obtained from the ABG analysis of the blood collected at the time of admission while the patient is awake, reflects the PaCO2 during sleep, we estimated the PaCO2 level during sleep using the prediction formula for PaCO2 at rest including during sleep (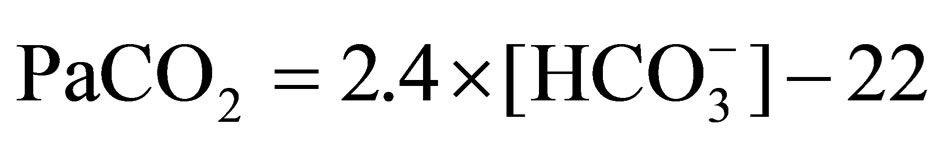 ) [18].
) [18].
Using this data, the subjects were classified into High PaCO2 and Normal PaCO2 Groups and compared. The results showed prolonged sleep latency in the High PaCO2 Group, for which intensified insomniac symptoms as in the previously mentioned COPD cases seemed to be a possible cause since the patients in this study all had severe respiratory failure.
Some reports suggest increase in Stage 1 observed in the group with OSAHS and hypercapnia as the cause of sleepiness. Continued arousal state due to decreased cerebral blood flow during sleep is also a possibility. Chemical, neurogenic, and myogenic controls function to modulate cerebral blood flow [30-32] and carbon dioxide is considered to affect the cerebral blood flow most [30]. A study by WollF [33] et al. and subsequent studies [34,35] confirm that increase in partial pressure of arterial CO2 dilates the cerebral blood vessel while the decrease contracts the vessel.
However, the mechanism concerning PaCO2 increase is yet to be confirmed since there are two opinions at the moment: relaxation of the smooth muscle in the cerebral blood vessel due to a chemical mechanism [36,37] and cerebral blood flow increase via neuroreflex [38]. Regarding the influence of PaCO2 on LTOT patients, it is conjectured that decrease in ventilation increases PaCO2 partial pressure, which dilates the cerebral blood vessel and increases cerebral blood flow resulting in the volume of cerebral blood flow equal to or larger than the flow during wakefulness. However, the possibility of prolonged sleep latency and decrease in TST was suggested. It may be necessary to take actual PaCO2 during sleep using the non-invasive method of measuring carbon dioxide concentration, classify the patients by the values, and make comparisons.
Prolonged sleep latency, shortened sleep time and decreased deep sleep were found in CRF patients with hypercapnia even with exclusion of the influence of hypoxia, which suggested the possible influence of CO2.
This study did not measure PaCO2 directly during sleep. Because there is a possibility that the collection of ABG sample during sleep can affect sleep architecture. This is regarded as major limitations of this study. It will be also examined sleep architecture after the intervention with assisted ventilation.
In conclusions, maintaining a certain oxygen level during sleep may not be sufficient to achieve adequate sleep in CRF patients with hypercapnia under LTOT.
Abbreviations
Long-term oxygen therapy (LTOT);
Chronic obstructive pulmonary disease (COPD);
Chronic Respiratory Failure (CRF);
Arterial blood gas analysis (ABG);
Polysomnography (PSG);
Total Sleep Time (TST);
Periodic leg movement disorder (PLMD).
NOTES