Placentas and Newborns of Patients Suffering from High Blood Pressure in University Hospital of Brazzaville ()
1. Introduction
As a mother-fetus interface, the placenta ensures the gaseous and nutritive exchanges required for growth and fetal development. Simple anatomical waste having accomplished its work of nutrition in our societies is endowed with a mystical power protector. It is often burned, thrown, or buried [1] [2] . Its development undergoes continuous morphological and functional changes, and it interacts with the mother and the fetus [1] [2] . Examination of the placenta is not systematic in the context of high blood pressure in our hospital [3] . The present work aims to contribute to the management of patients with hypertension by analyzing placenta.
2. Patients and Methods
This is a case-control study conducted from 1 January to 31 October 2017 in the University Hospital of Brazzaville (birth room, Laboratory of Pathological and Anatomy) and in the Faculty Health Sciences (laboratory of Anatomy and Organogenesis). The study concerned 40 placentas delivered and neonates of hypertensive patients compared to 40 of non-hypertensive patients. Placentas and neonates born from fetal pregnancies with at least 28 weeks of amenorrhoea with or without hypertension were included in the study. Incomplete, abnormally inserted or adhered placentas and scar uteri of both populations were not taken into account. Recruitment of placentas and newborns was performed by random draw according to the ratio of placenta and neonate of a hypertensive to that of a non-hypertensive birth that followed directly.
The procedure for examining the placenta was as follows:
- Immediate collection of the placenta and transport to the laboratory of anatomy and organogenesis for a morphological study
- Wash the placental vascular network with physiological saline to get rid of blood clots and staining the umbilical vessels for a reconstitution of the placental vascular tree;
- Macroscopic examination of the placenta after immersion of the placenta in 10% formalin and dissection by 5 mm serial sections;
- Histological examination after identification, dehydration, paraffin embedding and hematoxylin-eosin staining.
The colored cups were finally protected by a glass slide mounted with the balm of canapa.
The variables studied were maternal (age, parity and type of arterial hypertension), placental (shape, measurements, constitution, vascularization, and microscopy), and neonatal (term, weight, Apgar score) and transfer to neonatology).
The comparison of percentages used the Chi-square test and that of the averages the t-Student test. The value of p < 0.05 was considered as a threshold of statistical significance.
Cette étude a reçu l’accord du comité d’éthique.
Conflit d’intêret aucun.
3. Results
Patients were similar in age (26.9 ± 1.2 years VS 26.5 ± 1.1 years, p = 0.17) and parity (1.26 ± 0.7 VS 1, 61 ± 0.3, p = 0.26). The type of hypertension in the cases returned to pre-eclampsia (68%), pregnancy (20%), and chronic (12%).
The form of the placentas with HBP was similar to that of non HBP patients: circular (65.5% VS 67%, p = 0.65) and oval (34.5% VS 33%, p = 0.65).
A significant reduction in placenta measurements was observed more in hypertensives weight (431 ± 37 g VS 503 ± 26 g, p < 0, 05), diameter (17.40 ± 1.2 cm VS 19.25 ± 1 cm, p < 0.05), and area (239.82 ± 15.7 cm2 VS 292.1 ± 22.2 cm2, p < 0.05) as reported in Table 1. The umbilical cord of different term (37.07% ± 2.19% VS 38.41% ± 0.93%, p = 0.001).
Macroscopic placental lesions (Table 2) were represented by calcifications (75% VS 43.8%, p < 0.05) and the retro placental hematoma cup (18.8%) among the cases. Microscopic lesions were more observed in hypertensives: infarction (68.8% VS 18.8%, p = 0.004) and endarteritis (93.8% VS 12.5%, p < 0.05) and the cup of retro placental hematoma in cases. Microscopic lesions of villous hyalinosis (Picture 1) and endarteritis were more observed in hypertensive patients. Other microscopic lesions such as villous haemangioma (Picture 2) and chondroid metaplasia (Picture 3) were observed exclusively in hypertensive patients.
The characteristics of the newborns were different between the two populations: the term, the weight, the APGAR score, and the transfer to neonatology (Table 3).
4. Discussion
The retrospective nature of the study did not allow us to establish the link between the types of hypertension, placental involvement on the one hand and neonatal repercussions on the other.
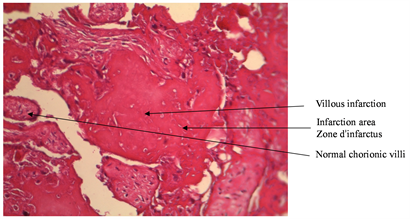
Picture 1. (HE) Gx300 Villous hyalinosis.

Picture 2. (HE) Gx300 Villous Hemangioma.
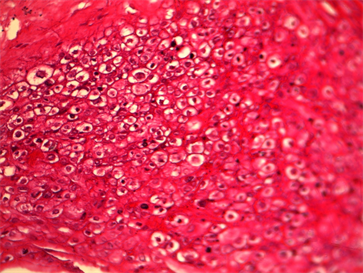
Picture 3. (HE) Gx300 Chondroid Metaplasia.
![]()
Table 1. Placental form and measurement.
![]()
Table 3. Characteristics of newborns.
IUGR: intra uterine growth retardation.
However, like Segupta [4] in Bangladesh, we did not find any difference between the ovular and circular forms of placentas of hypertensives and non-hypertensives.
On the other hand arterial hypertension has led to an overall reduction in placental measurements including weight, diameter, surface, thickness and volume. Similar results have been reported by other authors [5] [6] [7] [8] [9] who reveal that the pathological process is related to vascular involvement, which interferes with normal placental growth by reducing intakes.
Thus macroscopically abnormalities of the placental and funicular vascular architecture observed would promote vascular rupture and could explain the existence of the cup of retro placental hematoma (RPH) exclusively in the hypertensive population. Our results corroborate those of Pasricha [10] who found RPH in 33% of placentas only in hypertensive patients.
In contrast, thrombotic occlusion of placental uterine vessels may occur and explain the more frequent placental infarction in hypertensive patients. These results are similar to those of Udaina [11] , who in 2004 reported 92.5% of placental infarction from hypertensives against 29%, and emphasized that an attack greater than 5% of the placental surface is considered as being pathological.
Similarly the rate of increased placental calcifications in hypertensives was reported by Pasricha [10] in 70% of hypertensive placentas compared to 10% in the control group. These results suggest that HBP by its perfusion abnormalities would cause placental stress at the origin of early maturation.
Microscopically, endarteritis, which is the inflammation of the inner layer of the artery, was found mainly in the HBP group. These results are close to those of the literature [11] [12] [13] [14] . The consequences that result from this inflammation are either obliteration of the vascular lumen or clot formation due to the modification of the endothelial structure.
The various macroscopic and microscopic lesions resulted in an alteration of the placental exchange functions that may resonate on the fetus. Thus our study revealed a prevalence of hypotrophy close to that of Prabhjot [5] , who found 44% of hypotrophy exclusively in pre-eclampsia. Hypertensive newborns had a poor Apgar rating following perinatal asphyxia with a higher neonatal transfer.
5. Conclusion
This work confirmed the repercussions of high blood pressure on the placenta and the newborn. Examination of the placenta is therefore of interest in understanding perinatal pathology.